Percutaneous extraction of cement leakage after vertebroplasty under CT and fluoroscopy guidance: a new technique
We report on a new minimally invasive technique of extraction of cement leakage. Seven patients treated for vertebral compression fractures by percutaneous vertebroplasty had cement leakage into perivertebral soft tissues. Immediately following the vertebroplasty, percutaneous extraction was performed using an endoscopy clamp under CT and fluoroscopy guidance. In each patient, all cement fragments were withdrawn within ten minutes, without complication. This report suggests that this percutaneous technique could allow to reduce the rate of cement leakage-related complications.
Key Words: Vertebroplasty; Polymethylmethacrylate; Extraction of cement leakage; CT and fluoroscopy guidance; Interventional radiology.
Introduction
Percutaneous vertebroplasty was first performed by Galibert and Deramond in 1984 [1]. The procedure is now widely used for many painful vertebral compression fractures which may be secondary to osteoporosis, metastatic tumors, multiple myeloma and hemangioma [2, 3]. Complications are rare, and most are related to cement leakage into the spinal canal or the perivertebral venous system [4-6].
Many technical improvements including better procedure preparation, needle placement and cement injection have been made to reduce the incidence rate of cement leakage [7-9]. However, to the best of our knowledge, no study using a percutaneous technique has ever been published about the extraction of cement leakage to avoid its local complications.
We report on a new minimally invasive technique using computed tomography (CT) and fluoroscopy guidance to retrieve immediately after vertebroplasty cement leakage which was located into the paraspinal soft tissues along needle route.
Technique
Patients
From January 2008 to November 2010, more than 1500 percutaneous vertebroplasties were performed in our department of radiology to treat painful vertebral compression fractures secondary to osteoporosis, osteolytic metastases, multiple myeloma, painful or aggressive hemangioma.
All patients were treated by a senior interventional radiologist (with ten years of experience).
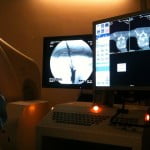
After haemostatic control, procedures were performed under surgical conditions of aseptia in an interventional CT room using CT (GE Lightview 8-row MDCT scanner; GE Healthcare, Waukesha, Wis, USA) and lateral fluoroscopy (GE Stenescop C-arm) guidance. The first part of the intervention was a CT acquisition centered around the fractured vertebra. Millimetric multiplanar reconstructions were analyzed on a GE ADW 4.2 workstation to confirm the diagnosis and plan the approach. An imaginary line of the needle trajectory passing through the center of the vertebra was drawn on the CT image for guidance. A skin entry point was determined, and the distance was measured from the midline.
Radiopaque markers were put on the skin prior to the insertion of the hardware. Using a 20-gauge 20-cm Chiba needle (Cook Medical, Bloomington, IN, USA), local anesthesia (lidocaïne 1% [Xylocaïne; Astra, Sodertalge, Sweden]) was administered from subcutaneous tissues to bone contact under fluoroscopy guidance. A CT acquisition confirmed the correct positioning of the tip of the needle. After its hub had been removed, the Chiba needle was then used as a guide for a 13-gauge 10-cm Trocar t’am (Thiebaud, Thonon-les-Bains, France) which was placed to the center of the fractured vertebra under CT and fluoroscopy guidance.
Polymethylmethacrylate (PMMA) cement mixed with tungsten powder (4 g) to increase its radiopacity was injected intravertebrally under dual guidance. The mean volume of cement ± standard deviation (SD) which was infused to fill each vertebra was 5.0 ± 1.0 mL.
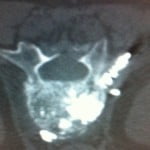
The CT scan of the treated vertebrae performed at the end of the procedure identified cement leakage along needle route into paraspinal soft tissues in seven patients (Fig. 1). Five patients were women and two were men, and the mean age ± SD was 81 ± 6 years (range, 68-88 years). These patients were treated for painful vertebral compression fractures that were secondary to osteoporosis (n = 5) and multiple myeloma (n = 2). Vertebroplasty was performed on the following vertebrae: D12 (n = 2), L1 (n = 3), L2 (n = 1) and L3 (n = 1), using a single posterolateral (laterovertebral or intercostovertebral) route.
Technique of extraction
Only a few minutes after the end of the vertebroplasty (corresponding to the time necessary for the setting of the cement), the procedure of extraction was performed under surgical conditions of aseptia and local anesthesia (lidocaïne 1% [Xylocaïne; Astra, Sodertalge, Sweden]). A 20-gauge Chiba needle (Cook Medical, Bloomington, IN, USA) was first inserted using the same route as the vertebroplasty under fluoroscopy until contact was obtained with the cement fragment.
This needle was then used as a guide for an 11-gauge 10-cm Trocar t’am (Thiebaud, Thonon-les-Bains, France) which was inserted under fluoroscopy after the hub had been removed.
A CT scan was acquired to confirm the correct positioning of the cannula in relation to the guidewire.
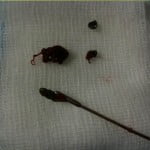
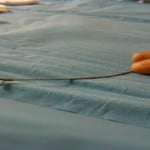
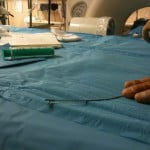
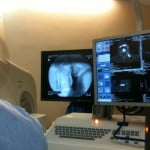
Following needle withdrawal, a 13-gauge endoscopy clamp (Meditech, Watertown, MA, USA) was inserted through the cannula of the Trocar to extract the cement fragment under fluoroscopic guidance (Figs 2 and 3). This last step was repeated if several fragments (n ≤ 5) were present. For each case, all cement fragments were successfully withdrawn during the same procedure (Fig. 4).
A CT scan was lastly performed to check the removal of all cement framents.
Procedural time was approximately 10 min.
No complication was observed during or following the procedure.
Discussion
Percutaneous vertebroplasty is an interventional radiologic procedure that involves an injection of acrylic bone (PMMA) cement into a diseased vertebral body under fluoroscopy and/or CT guidance. The first percutaneous vertebroplasty of which we are aware was performed in France in 1984 and reported in the literature in 1987: Galibert et al. [1] injected PMMA into the C2 vertebra, which had been partially destroyed by an aggressive hemangioma. Since that, vertebroplasty has gained widespread popularity for the treatment of painful vertebral compression fractures which may be secondary to osteoporosis, osteolytic metastases and multiple myeloma [2, 3].
During vertebroplasty procedures, cement leakage is common and mostly asymptomatic. It may nevertheless lead to local or systemic complications. The main systemic complication is pulmonary cement embolism caused by PMMA migration into the perivertebral venous plexuses during this procedure [5].
The most serious local complication is spinal cord compression due to epidural overflow of PMMA [6]. The second neurological complication is radiculopathy caused by PMMA leakage into the neural foramen [4]. Cement may also leak into paraspinal soft tissues, intervertebral disk or adjacent joint areas [10, 11]. Paraspinal cement leakage (like in our report) can cause radiculopathy due to the presence of cement into the extraforaminal space impinging on nerve root, and requiring surgery [12]. Moreover, another complication of paraspinal cement leakage is subsequent infection including an abscess, which may require medical, interventional or surgical treatment [10].
To avoid cement leakage-related complications, meticulous techniques have been developed in all steps of the vertebroplasty procedure. First, the viscosity of the PMMA is a crucial point during the intervention, and progressively increases as a result of methyl methacrylate polymerization. The rate of polymerization depends on several factors including the ambient temperature and the quantity of the solvent. A paste is preferred to a liquid consistency because the latter may cause migration into the venous system [5]. Anselmetti et al. [13] showed also that high-viscosity PMMA allowed a significant reduction of extravasation rate and consequently leakage-related complications. Second, an adequate amount of PMMA is also recommended. Indeed, Martin et al. [14] reported that complications could be related to an excessive PMMA injection. Third, good-quality imaging guidance is essential for the early detection of a minimal cement leakage into the perivertebral veins. Excellent opacification of cement with radiological contrast material (in our case, tungsten) is essential for the early detection of venous migration of cement [1, 15]. Moreover, in a study by Gangi et al. [8], vertebroplasty procedures were guided by the combination of CT and fluoroscopy, which allowed to facilitate needle placement and thus to reduce the occurrence of cement. But despite the use of this dual guidance like in our case, real-time detection of laterovertebral leakage remains difficult owing to the overlap of the cement filling vertebral body. Biplanar fluoroscopy could be used to overcome this problem [15].
Since its first description more than four decades ago [16], the percutaneous retrieval of intravascular foreign bodies has become a frequently applied technique. The rapid development and wide application of minimally invasive and interventional techniques have been associated with an increased rate of specific method-related complications caused by intravascular foreign bodies [17]. Many devices (such as snares, biopsy forceps, Dormia baskets or tip-deflecting wires) have been used to retrieve various types of intravascular objects.
The percutaneous removal of foreign bodies was expanded to visceral procedures. O’Shea et al. [18] described a minimally invasive technique used to remove calculi from the peritoneal cavity which had been retained after surgery. Ojanguren et al. [19] also reported on a percutaneous method which allowed to withdraw retained T-tubes without complication.
More recently, in musculoskeletal interventional radiology, CT and fluoroscopy guidance was used to percutaneously withdraw surgical pin fragments that had accidentally migrated into the soft tissues of two patients’shoulders [20]. Our minimally invasive procedure of cement extraction performed immediately after vertebroplasty under only local anesthesia confirms the crucial role of dual guidance, making the intervention rapid, safe and effective.
In conclusion, this report of a few cases suggest that this percutaneous technique could allow to avoid the potential local complications of cement leakage into the paraspinal soft tissues (such as radiculopathy or infection). Moreover, it could be interesting to try to extend this procedure to the foramen in which the risk of nerve root compression by cement leakage is high, requiring in such cases surgery.
References
1. Galibert P, Deramond H, Rosat P, Le Gars D. (1987) [Preliminary note on the treatment of vertebral angioma by percutaneous acrylic vertebroplasty]. Neurochirurgie 33(2):166-168.
2. Barragan-Campos HM, Vallee JN, Lo D, et al. (2006) Percutaneous vertebroplasty for spinal metastases: complications. Radiology 238(1):354-362.
3. Cotten A, Dewatre F, Cortet B, et al. (1996) Percutaneous vertebroplasty for osteolytic metastases and myeloma: effects of the percentage of lesion filling and the leakage of methyl methacrylate at clinical follow-up. Radiology 200(2):525-530.
4. Kelekis AD, Martin JB, Somon T, Wetzel SG, Dietrich PY, Ruefenacht DA. (2003) Radicular pain after vertebroplasty: compression or irritation of the nerve root? Initial experience with the “cooling system”. Spine (Phila Pa 1976) 28(14):E265-269.
5. Padovani B, Kasriel O, Brunner P, Peretti-Viton P. (1999) Pulmonary embolism caused by acrylic cement: a rare complication of percutaneous vertebroplasty. AJNR Am J Neuroradiol 20(3):375-77.
6. Teng MM, Cheng H, Ho DM, Chang CY. (2006) Intraspinal leakage of bone cement after vertebroplasty: a report of 3 cases. AJNR Am J Neuroradiol 27(1):224-229.
7. Basile A, Cavalli M, Fiumara P, et al. (2011) Vertebroplasty in multiple myeloma with osteolysis or fracture of the posterior vertebral wall. Usefulness of a delayed cement injection. Skeletal radiology 40(7):913-919.
8. Gangi A, Kastler BA, Dietemann JL. (1994) Percutaneous vertebroplasty guided by a combination of CT and fluoroscopy. AJNR Am J Neuroradiol 15(1):83-86.
9. Jin YJ, Yoon SH, Park KW, et al. (2011) The volumetric analysis of cement in vertebroplasty: relationship with clinical outcome and complications. Spine (Phila Pa 1976) 36(12):E761-772.
10. Lee IJ, Choi AL, Yie MY, et al. (2010) CT evaluation of local leakage of bone cement after percutaneous kyphoplasty and vertebroplasty. Acta Radiol 51(6):649-654.
11. Lin EP, Ekholm S, Hiwatashi A, Westesson PL. (2004) Vertebroplasty: cement leakage into the disc increases the risk of new fracture of adjacent vertebral body. AJNR Am J Neuroradiol 25(2):175-180.
12. Chen JK, Lee HM, Shih JT, Hung ST. (2007) Combined extraforaminal and intradiscal cement leakage following percutaneous vertebroplasty. Spine (Phila Pa 1976) 32(12):E358-362.
13. Anselmetti GC, Zoarski G, Manca A, et al. (2008) Percutaneous vertebroplasty and bone cement leakage: clinical experience with a new high-viscosity bone cement and delivery system for vertebral augmentation in benign and malignant compression fractures. Cardiovasc Intervent Radiol 31(5):937-947.
14. Martin JB, Wetzel SG, Seium Y, et al. (2003) Percutaneous vertebroplasty in metastatic disease: transpedicular access and treatment of lysed pedicles–initial experience. Radiology 229(2):593-597.
15. Jensen ME, Evans AJ, Mathis JM, Kallmes DF, Cloft HJ, Dion JE. (1997) Percutaneous polymethylmethacrylate vertebroplasty in the treatment of osteoporotic vertebral body compression fractures: technical aspects. AJNR Am J Neuroradiol;18(10) 1897-1904.
16. Thomas J, Sinclair-Smith B, Bloomfield D, Davachi A. (1964) Non-Surgical Retrieval of a Broken Segment of Steel Spring Guide from the Right Atrium and Inferior Vena Cava. Circulation 30:106-108.
17. Gabelmann A, Kramer S, Gorich J. (2001) Percutaneous retrieval of lost or misplaced intravascular objects. AJR Am J Roentgenol 176(6):1509-1513.
18. O’Shea SJ, Martin DF. (2003) Percutaneous removal of retained calculi from the abdomen. Cardiovasc Intervent Radiol 26(1):81-84.
19. Ojanguren A, Doenz F, Qanadli SD, et al. (2005) Percutaneous extraction of retained biliary T-tubes: a new technique. J Vasc Interv Radiol 16(7):1033-1036.
20. Amoretti N, Hauger O, Marcy PY, et al. (2010) Foreign body extraction from soft tissue by using CT and fluoroscopic guidance: a new technique. Eur Radiol 20(1):190-192.
Figure captions
Figure 1. The CT scan performed at the end of the vertebroplasty procedure identified cement leakage into the paraspinal soft tissues.
Figure 2. A 13-gauge endoscopy clamp (Meditech, Watertown, MA, USA)
Figure 3. Removal of a cement fragment using an endoscopy clamp under fluoroscopic guidance.
Figure 4. Four cement fragments which were withdrawn.