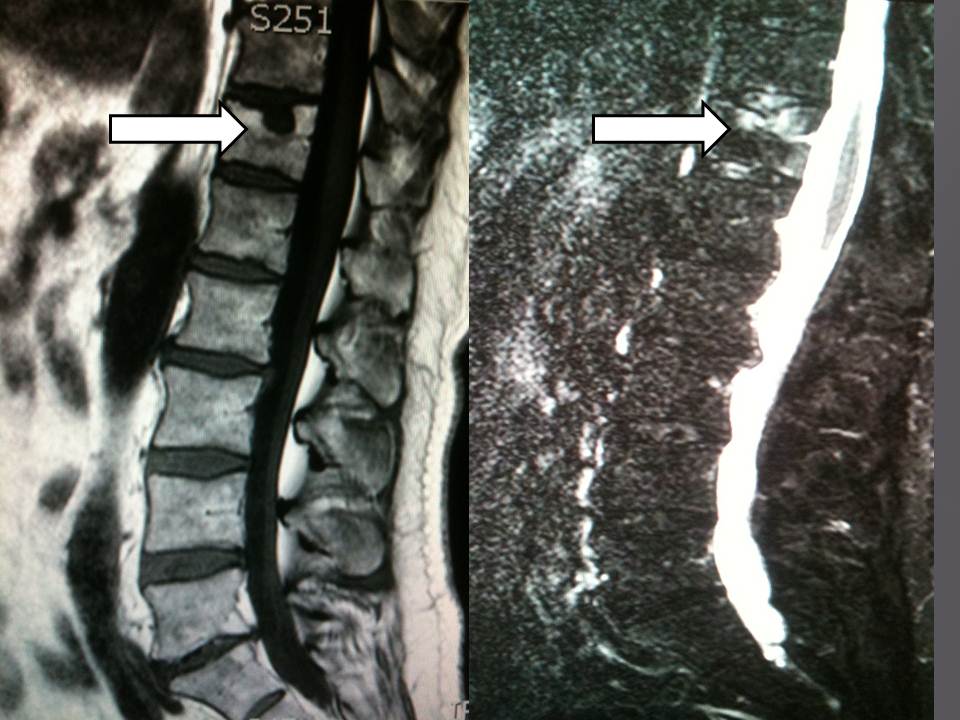
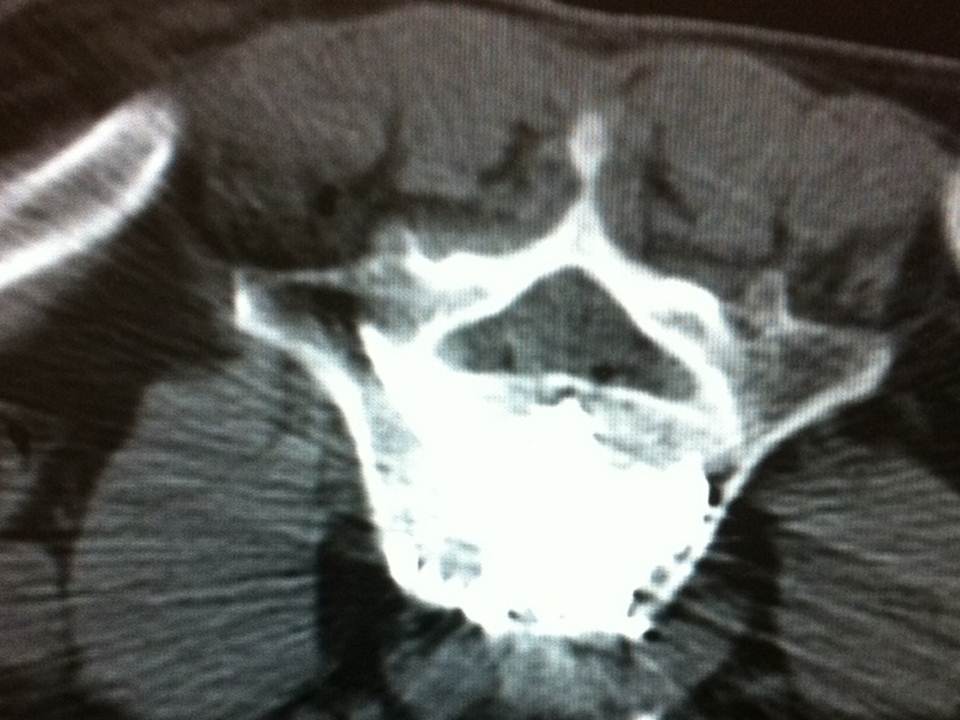
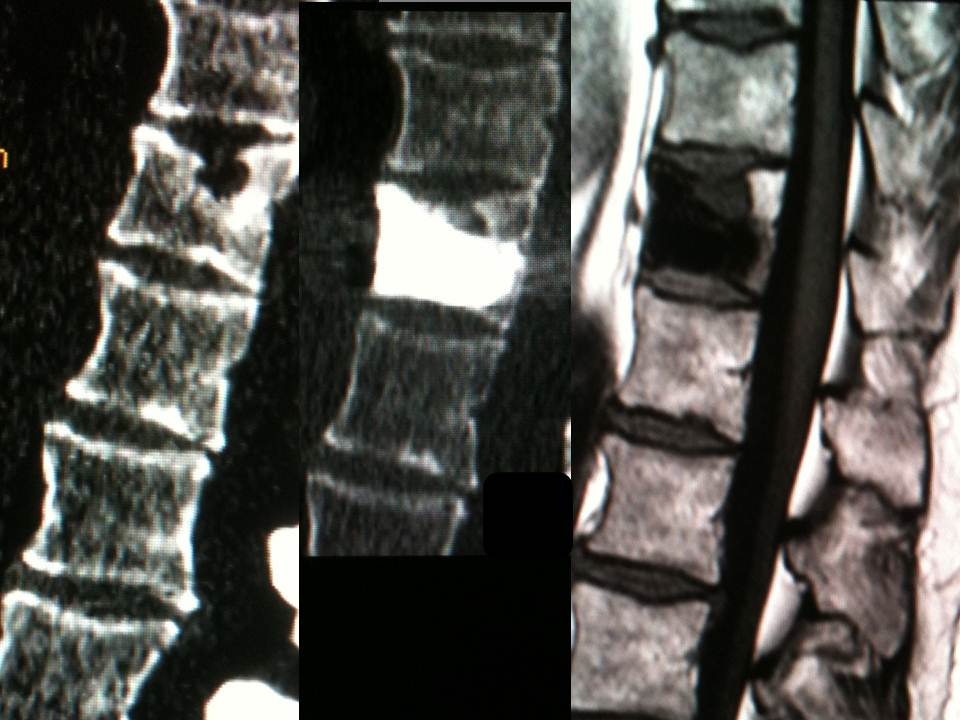
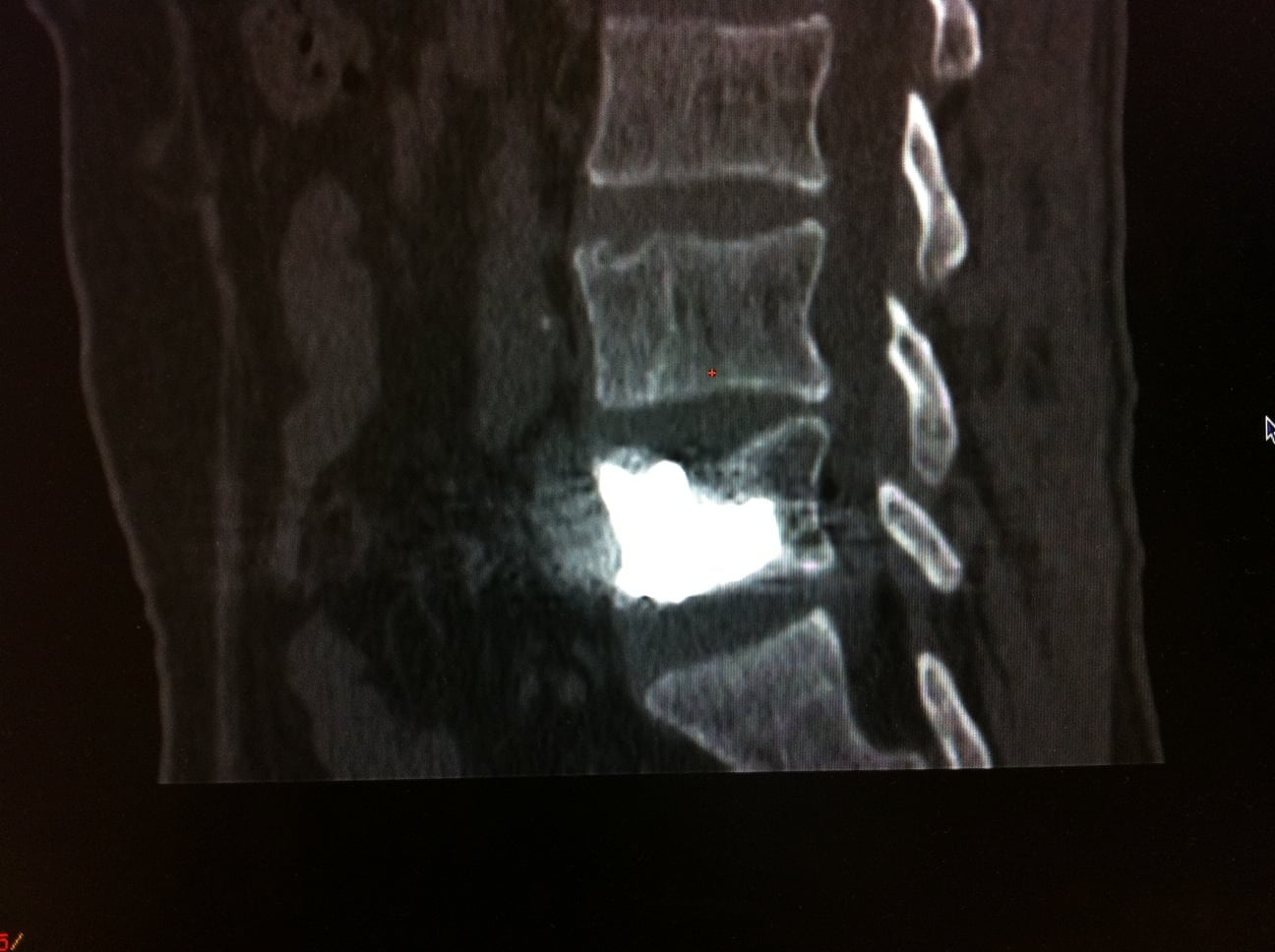
- MRI is necessary to analyze the vertebral level to treat and shows increased intensity in the bone marrow surrounding the hernia
Symptomatic schmorl nodes : role of percutaneous vertebroplasy.
open study on 52 consecutives patients
Abstract
Objective
The aim of this study was to evaluate CT- and fluoroscopy-guided percutaneous vertebroplasty in the management of painful Schmorl node.
Materials and Methods
Monocentric prospective study was carried out between (January2007 to January2010) for 52 consecutive patients who were managed by CT Guided percutaneous vertebroplasty for symptomatic schmorl hernia (back pain for at least 6 months). 22 men and 30 women with an age varying from 42y to 88years old were treated. A clear consent was signed by all patients and the study was approved by IRB of our university. The pain due to the fracture was evaluated between (6 to 10) with an average scale of 7.2 according to VAS
Results
The results obtained match those of the literature in the area of painful osteoporotic fractures.52 patients and 52 vertebra were treated. Vertebroplasty procedures vary from 15 to 27 minutes, with an average of 22 minutes from the arrival to the departure of the patient. The vertebra filling was satisfactory in all cases. The cement volume injected varied between 2cc to 5cc. The VAS and Oswetry disability index decreased from 7.2+/- 1.5 to 2.1 +/- 1.0 and from 59.2+/- 16.2 to 17.1 +/- 5.0 respectively. All the results were stable in time particularly long term 1 follow-up.
Conclusion
The results of our study showed that painful schmorl node could be successfully treated by a percutaneous vertebroplasty under CT and fluoroscopic guidance with an excellent long-term outcome. The brief hospitalization and the speedy return to active life have very interesting economic and social consequences.
Keywords: Vertebroplasty. Schmorl node.Local anesthaesia. CT and fluoroscopy guidance. Interventional radiology
Percutaneous vertebroplasty was first performed by Deramond in 1984 at the Amiens Centre Hospitalier Universitaire in France. It consists in the injection of acrylic cement in the vertebral body to reinforce it. The first indication was an aggressive angioma (1-2). Indications have been extended to metastatic vertebral state and to hyperalgic osteoporotic fractures. The evolution of material and experience of operators allowed for an expansion of the use to traumatic fractures and metastatic vertebrae reaching corticals (3-11).
Schmorl nodes represents disc herniations into vertebral bodies. Conservative treatment is generally sufficient in patients with back pain. Painful Schmorl nodes refractory to medical therapy should be a new indication of percutaneous vertebroplasty. Few articles have study the effect of a percutaneous consolidation in the case of symptomatic schmorl hernia (12-13).The objective of this article is to present the role of Vertebroplasty in the case of painful Schmorl nodes.
Material and methods:
Monocentric prospective study was carried out between (January2007 to January2010) for 52 consecutive patients who were managed by CT Guided percutaneous vertebroplasty for symptomatic schmorl hernia (back pain for at least 6 months). 22 men and 30 women with an age varying from 42y to 88y old (an average age of 78 years old) were treated. A clear consent was signed by all patients and the study was approved by IRB of our university. The pain due to the fracture was evaluated between (6 to 10) with an average scale of 7.2 according to VAS. The patients had complete functional impotence regarding their immobility status. The indication was proposed according to an interdisciplinary meeting of interventional radiologists and orthopedics.
Preprocedural radiological findings confirmed the presence of painful Schmorl nodes in absence of other causes of back pain, such as herniated intervertebral disc, body vertebral fracture, or body malignant lesions.
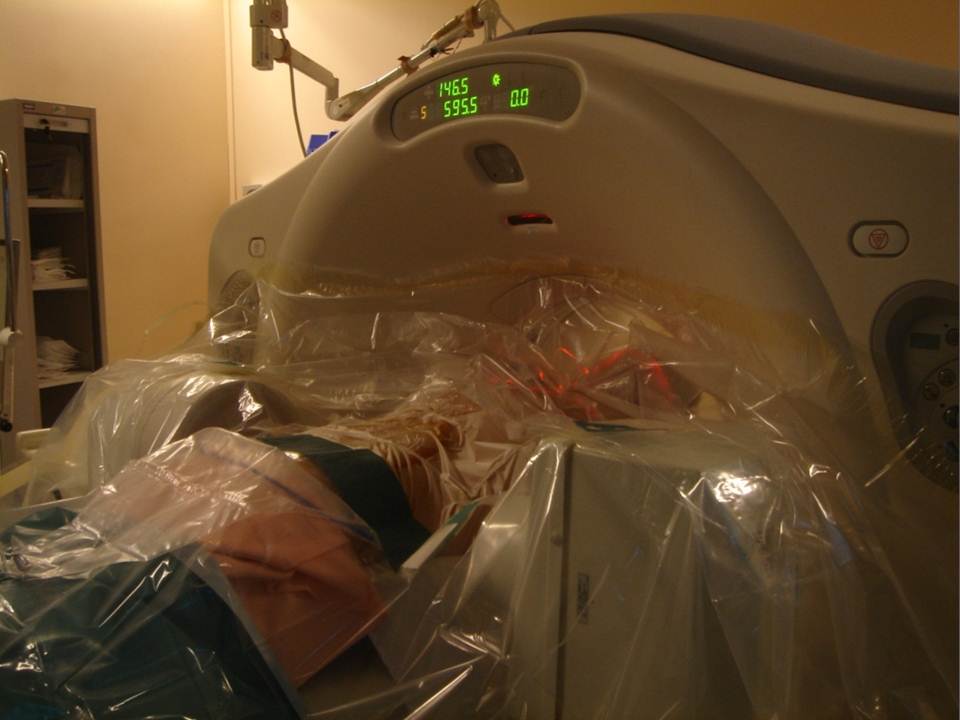
A preliminary MRI is necessary to analyze the vertebral level to treat, by visualization of a vertebral hypersignal in weighted sequence in T2 with fatty signal cancellation showing a secondary edema at the bodily lesion, a fracture can be shown under the schmorl hernia confirming the pathogeny of the symptoms. MRI is a valuable aid both in evaluation of the location of Schmorl nodes and in the delineation of the amount of perilesional intraspongious suffering (Fig 1). A inflammatory discitis semeiology at the MRI is an exclusion criteria. The common feature of the cases presented here is the double scannographic and fluoroscopic guiding system which allows for easier trocar positioning with better visualization of vertebral structures and lesions and to control the vertebral filling in real time to limit cement leaks (14-15). All patients were treated by a senior interventional radiologist (with ten years of experience). After haemostatic control, procedures were performed under surgical conditions of aseptia in an interventional CT room using CT (GE Lightview 8-row MDCT scanner; GE Healthcare, Waukesha, Wis, USA) and lateral fluoroscopy (GE Stenoscop C-arm) guidance (Fig 2). The preparation of the material requires: a sterile table drape, a perforated sterile drape (used for angioplasties), a 22 gauges needle for under cutaneous anesthesia, 1% xylocain, a scalpel and two 13 gauges trocars for guided vertebroplasty and vertebral biopsy.
The patient is set in procubitus with a hyperlordosis ventral block. A volume acquisition on the whole rachis is performed. The multiplanar reconstruction allow for check of the level to treat and the way. The stone of the way is realized on the axial cuts allowing a tranpedicular approach, intercostal-vertebral of extra-vertebral depending on the level to treat. A radio-opaque point is positioned on the skin in function of the marks established on the axial cuts of the scanner and confirmed by a new acquisition.
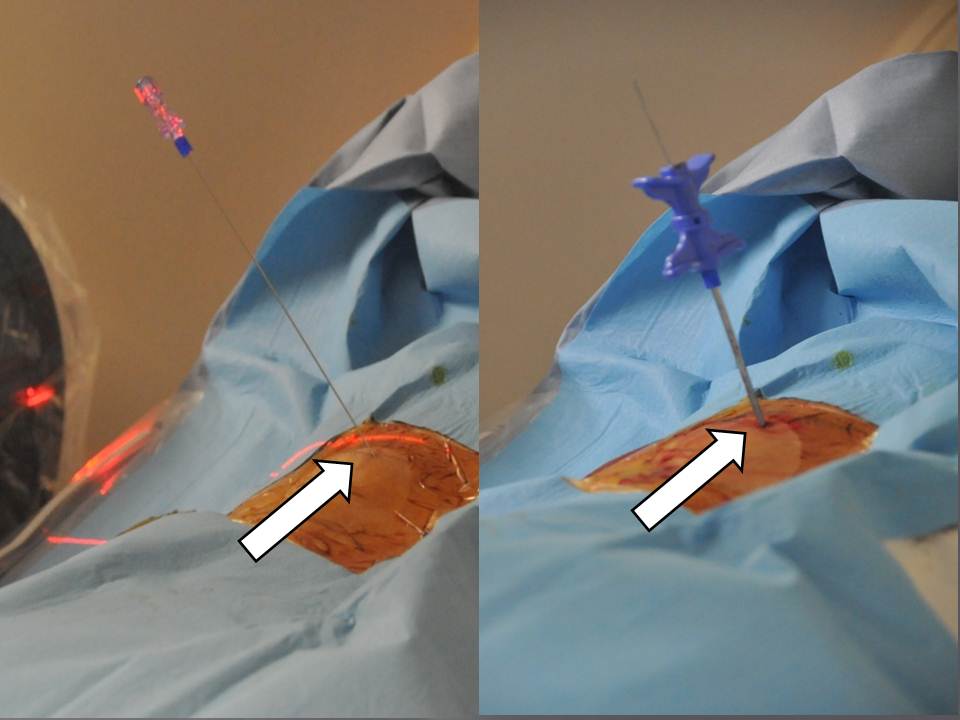
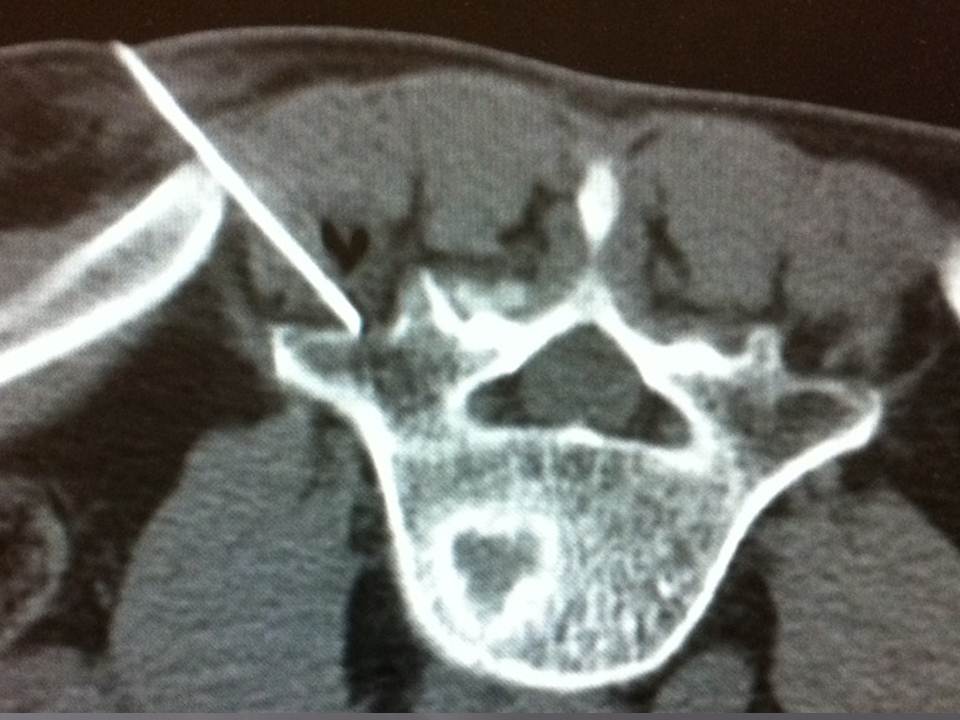
All the interventions are performed under local anesthesia according to the same protocol: the local anesthesia is performed by injecting 3 ml of 1% xylocain (lidocaïne 1% Xylocaïne; Astra, Sodertalge, Sweden), 3 min are enough before inserting the 20 gauges shiba needle 20 cm at the point of contact of the periost under scopic guide. A scanner control in step by step mode allows for confirmation of correct positioning of the shiba needle.Approximately 3 ml of 1% xylocain is again injected at the vertebral point of entry to perform the periosted anesthesia. The removable connector of the Shiba needle is pulled out, leaving space for a true guide on which the trocar perforates and inserts to the contact with the bone, in particular at the precise level of the anesthesia (t’am,Thiebaud, Thonon-les-Bains, France)(Fig 3). The progress of the trocar in the vertebral body is occurring under iterative scopic guidance. A scanner control can confirm the correct position of the distal end of the trocar at the level of the zone to treat. A biopsie is performed using the coaxial canulae.
The cement preparation is performed with a mixer in closed loop to avoid vapors. The 1 ml syringe’s luer lock are filled at the early liquid phase of the cement. We use a cement (Osteo-firm Radiopaque bone cement; Cook, Bloomington, IN, USA) radio-opaque in which we mix 4 g of tungsten to increase opacity. This high radio-opacity enables a perfect visualization during vertebral filling and represents an additional safety aspect. The cement must posses variable phases of viscosity in time from liquid to paste.
We fill a first part of the vertebrae with a few drops of liquid cement to judge and anticipate the positioning and the frequent discal leaks. Under continual scopy, we visualize a linear diffusion intra-vertebral of the cement. Then we wait a few minutes to allow polymerization and get a high viscosity cement that we will push slowly in the cannula with a needle. The large viscosity at the end of the procedure is a key element to the correct filling of these fractures. The injection can be performed by filling the canulae and pushing the cement with the trocar. A thick and old cement diffuses close to the distal end of the trocar. Similarly the progressive retreat of the trocar by pushing to the needle the rest of the cement allows for perfect cementing in the rest of the way.
The subchondral space must be perfectly filled, the pressure in this space being smaller, the diffusion is easy. The post-operation precautions are the same as for osteoporotic fractures.
Results:
The results obtained match those of the literature in the area of painful osteoporotic fractures .52 patients and 52 vertebra were treated.Vertebroplasty procedures vary from 15 to 27 minutes, with an average of 22 minutes from the arrival to the departure of the patient.The vertebra filling was satisfactory in all cases. The cement volume injected varied betwenn 2cc to 5cc (m:2.8).DLP varied between 500 to 1620 mGy.cm (m:827).No neurological or infectious sequences were noted.We saw 7 discal leakages (6,7%) without any consequences on clinical evolution of the vertebra above and below.
A clinical and radiological follow-up is done 2 days, then 1 month, 6 months and 1 year after.
The VAS and Oswetry disability index decreased from 7.2+/- 1.5 to 2.1 +/- 1.0 and from 59.2+/- 16.2 to 17.1 +/- 5.0 respectively. All the results were stable in time particularly long term 1 and 2 years. (VAS of Huskisson: visual analog scale, a pain score with points assigned subjectively from patients preprocedure and postprocedure in a range between 0 (absence of pain) and 10 (maximum pain))
Discussion:
The schmorl hernia can be painful in some cases, this situation can occur when a collapse of the spongy bone holding the upper disc and able to provoke a large bone edema under chondral tissues. The principle of the vertebroplasty consists in consolidating the portion of the bone below the intra spongy hernia. The indication and the results of the consolidation of the vertebrae in this kind of bone damage has already been published (12-13) and showed a significant enhancement of the analog pain scale at the first day.
The vertebroplasty technique in this context can present a unique difficulty: the precision of positioning of the cement adjacent to the hernia with intra-discal passage. The scannographic volume acquisition determines in a first step the ideal path for the distal end of the trocar is located under the median portion of the hernia. The filling of the spongy bone is performed with a viscous cement which will fill the whole lower part to the hernia. The injection will be performed under continuous scopy and will avoid any disc passage. The rotation motions of the cannula bevel of the trocar can be very useful to better spread the cement.
The end of this mini invasive tecnic takes its true meaning when the intervention is associated to an efficient and well tolerated local anesthesia. Avoiding the general anesthesia and its complications.
The per-cutaneous vertebroplasty is an procedure that cannot be ignored in the therapeutic arsenal of the vertebral fracture in particular secondary to schmorl hernia.
The evolution of the material and the mode of guidance enable realization of this intervention in optimal conditions of safety and ease. Numerous expert centers chose this technical evolution for the clear enhancement of the tolerance of this procedure and the speed, ease and safety of the gesture.
Vertebroplasty is a good treatment for symptomatic intra-spongeous hernia when the inclusion and exclusion criterias are respected.
[toggle title=”REFERENCES: “]1.Galibert P, Deramond H, Rosat P, Le Gars D. Preliminary note on the treatment of vertebral angioma by percutaneous acrylic vertebroplasty.Neurochirurgie.1987;33(2):166-8
2. Franc J, Lehmann P, Saliou G, Monet P, Kocheida EM, Daguet E, Laurent A, Legars D, Deramond H. Vertebroplasty: 10 years clinical and radiological follow-up.J Neuroradiol. 2010 Oct;37(4):211-9
3. Fransen H. Minimal invasive treatment of vertebral compression fractures: vertebroplasty.Neuroradiology. 2011 Sep;53 Suppl 1:S199-201.
4. Muijs SP, van Erkel AR, Dijkstra PD. Treatment of painful osteoporotic vertebral compression fractures: a brief review of the evidence for percutaneous vertebroplasty.J Bone Joint Surg Br. 2011 Sep;93(9):1149-53
5. Klazen CA, Lohle PN, de Vries J, Jansen FH, Tielbeek AV, Blonk MC, Venmans A, van Rooij WJ, Schoemaker MC, Juttmann JR, Lo TH, Verhaar HJ, van der Graaf Y, van Everdingen KJ, Muller AF, Elgersma OE, Halkema DR, Fransen H, Janssens X, Buskens E, Mali WP. Vertebroplasty versus conservative treatment in acute osteoporotic vertebral compression fractures (Vertos II): an open-label randomised trial.Lancet. 2010 Sep 25;376(9746):1085-92
6. Brodano GB, Amendola L, Martikos K, Bettuzzi C, Boriani L, Gasbarrini A, Bandiera S, Terzi S, Greggi T, Boriani S. Vertebroplasty: benefits are more than risks in selected and evidence-based informed patients. A retrospective study of 59 cases.Eur Spine J. 2011 Aug;20(8):1265-71
7. Anselmetti GC, Manca A, Montemurro F, Hirsch J, Chiara G, Grignani G, Carnevale Schianca F, Capaldi A, Rota Scalabrini D, Sardo E, Debernardi F, Iussich G, Regge D.Percutaneous vertebroplasty in multiple myeloma: prospective long-term follow-up in 106 consecutive patients.Cardiovasc Intervent Radiol. 2012 Feb;35(1):139-45 2012
8. Saliou G, Kocheida el M, Lehmann P, Depriester C, Paradot G, Le Gars D, Balut A, Deramond H. Percutaneous vertebroplasty for pain management in malignant fractures of the spine with epidural involvement.Radiology. 2010 Mar;254(3):882-90.
9. Lee B, Franklin I, Lewis JS, Coombes RC, Leonard R, Gishen P, Stebbing J.The efficacy of percutaneous vertebroplasty for vertebral metastases associated with solid malignancies.Eur J Cancer. 2009 Jun;45(9):1597-602
10. Mont’Alverne F, Vallée JN, Guillevin R, Cormier E, Jean B, Rose M, Caldas JG, Chiras J.Percutaneous vertebroplasty for multiple myeloma of the cervical spine.Neuroradiology. 2009 Apr;51(4):237-42
11. McDonald RJ, Trout AT, Gray LA, Dispenzieri A, Thielen KR, Kallmes DF. Vertebroplasty in multiple myeloma: outcomes in a large patient series.AJNR Am J Neuroradiol. 2008 Apr;29(4):642-8
12.Masala S, Pipitone V, Tomassini M, Massari F, Romagnoli A, Simonetti G. Percutaneous vertebroplasty in painful schmorl nodes. Cardiovasc intervent Radiol 2006;29:97-101
13.Wenger M, Marwalder T. Fluoronavigation-assisted, lumbar vertebroplasty for painful Schmorl node. Journal of clinical Neuroscience.2009;1250-1251
12. Margel F, Aebi M, Gertzbein SD, Harms J, Nazarian S. A comprensive classification of thoracic and lumbar injurues. Eur Spine j.1994;3:184-201.
14. Gangi A(1994) Percutaneous vertebroplasty guided by a combination of CT and fluoroscopy.AJNR. Am J Neuroradiol. 15(1):83-6.
15. Amoretti N, Marcy PY, Lesbats-Jacquot V, Hovorka I, Fonquerne ME, Roux C, Hericord O, Maratos Y, Euller-Ziegler L.Combined CT and fluoroscopic guidance of balloon kyphoplasty versus fluoroscopy-only procedures.Skeletal Radiol. 2009 Jul;38(7):703-7[/toggle]